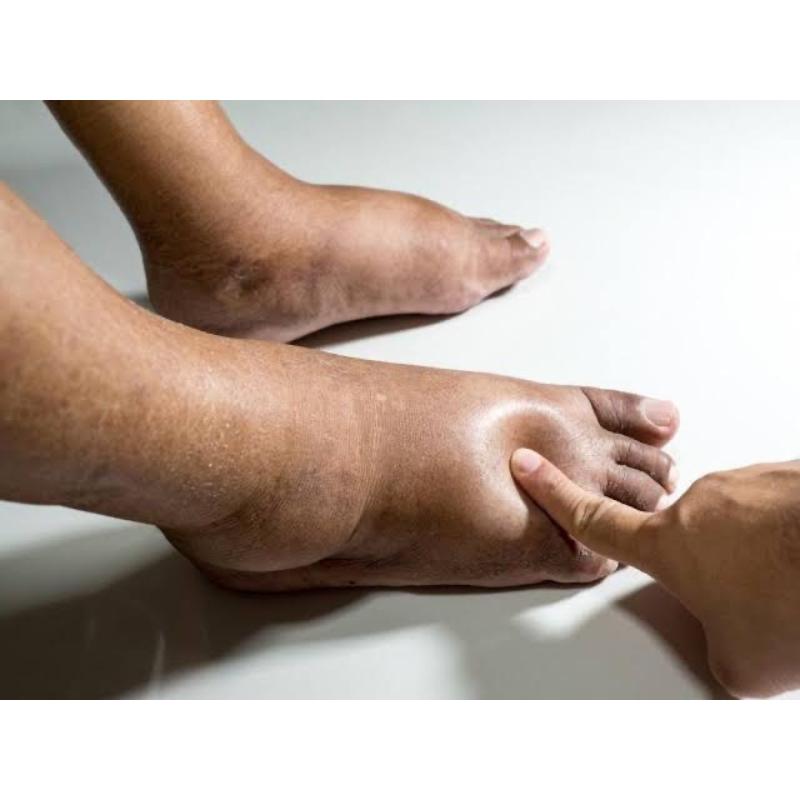
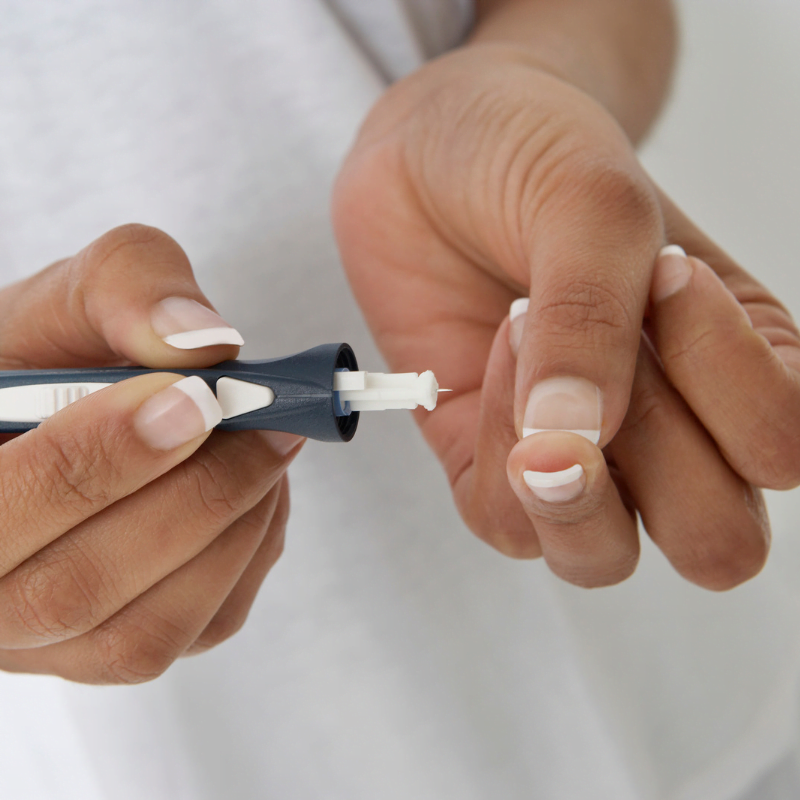
Diabetes also known as diabetes mellitus, is a group of common endocrine disease characterized by sustained high blood sugar level.
Diabetes is due to the pancreas not producing enough insulin or the cells of the body not responding properly to the insulin produced.
Diabetes affect people of all ages. Most forms of diabetes are chronic(long-life),and all forms are manageable with medications and/or life changes.
Glucose(sugar) mainly comes from carbohydrates in food and drugs. Its the body`s go-to source of energy. Your body carries glucose to all your body`s cell to use for energy. When glucose is in your blood stream, it needs assistance(a key) to get to where it needs to go. Insulin is the key, a hormone.
Hyperglycemia or high blood sugar, results from the blood stream`s accumulation of glucose which can happen if your pancreas doesn`t use it properly. Constantly high blood sugar levels over time can lead to health risks like heart disease, nerve damage and vision problems.
Types of Diabetes.
There four different types of diabetes, they include;
1)Type 1 Diabetes: Although it can occur at any age, this variety is typically identified in children, teenagers and young adults. In type 1 diabetes, the pancreas stops producing insulin. This implies that you must take insulin daily.
2) Type 2 Diabetes: This type can appear at any age, however it seems to occur more frequently in people over 40. when your body isn`t using the insulin properly your pancreas isn`t producing enough, type 2 diabetes develops.
3)Gestational Diabetes(diabetes in pregnancy): Some women experience this type of development when pregnant. After pregnancy, gestational diabetes typically disappears. The chance of acquiring type 2 diabetes in life is increased if you have gestational diabetes.
4)Prediabetes: This is the precursor type 2 diabetes. Although your blood glucose levels are above average they are not yet high enough to be given a type 2diabetes diagnosis.
Symptoms of Diabetes.
They include:
1)Dry mouth and increased thirst(polydipsia).
2)Urination on a regular basis
3)Fatigue.
4)Eye sight that is fuzzy.
5)Unexpected weight loss.
6)Numbness of the hand or feet.
7)Recurring yeast infections of the skin or vagina.
8)Wounds or sores that take a long time to heal.
9)Extremely dry skin.
Other symptoms that can occur with type 1 diabetes
-Nausea.
-Abdominal pain.
-Vomiting.
-Urinary tract infections or yeast infections.
Causes of Diabetes.
Diabetes, irrespective of the kind is caused by an excess of glucose in the blood. However, depending on the type of diabetes you have, there are several causes for elevated blood glucose levels.
Causes of diabetes include;
1) Insulin resistance: The main cause of type 2 diabetes is insulin resistance. Cells in your muscles, fat and liver become insulin resistant when they don`t react to insulin as it should. Insulin resistance is caused by a variety of illness and circumstances including obesity, inactivity, hormonal imbalance, heredity, and some drugs.
2) Autoimmune disease: When your immune system destroys the insulin producing cells in your pancreas, you can develop type 1 diabetes and latent autoimmune diabetes of adults(LADA).
3) Hormonal imbalance: The placenta releases substances that lead to insulin resistance through out pregnancy. If your pancreas can`t create enough insulin to overcome the insulin resistance, you can develop gestational diabetes. Acromegaly and cushings syndrome (two other hormone related disease) can also lead to type 2 diabetes.
4)Pancreatic damage: Your pancreas capacity to produce insulin may be impacted by a condition, surgery or injury, leading to type 3c diabetes.
5)Genetic mutations: Onset diabetes of the young (MODY) and neonatal diabetes may be caused specific genetic mutations.
Long term usage of several drugs, such as corticosteroids and Hiv/Aids treatment can result in type 2 diabetes.
Complications of Diabetes.
Possible complications include;
1)Kidney damage.
2)Eye damage.
3)Heart disease and problem.
4)Nerve damage(Neuropathy).
5)Foot damage.
6)lots of hearing.
7)Depression.
8)Dementia.
9)Dental problems.
10)Erectile dysfunction.
Other possible complications for women who have gestational diabetes include:
-High blood pressure.
-A higher risk of developing gestational diabetes into future pregnancies.
-A higher risk of developing type 2 diabetes in the future.
Diagnosis of Diabetes.
1)Fasting blood glucose test: For this test you must fast for eight hours the previous evening before having blood drawn the following morning. Fasting blood glucose levels below 100mg/dl are considered normal. Prediabetes is indicated by a reading between 100 and 125mg/dl.
Diabetes is indicated if your level is 126mg/dl or greater. As food can greatly affect blood sugar, this test allows your provider to see your base line blood sugar.
2)Random blood glucose test: You can perform this blood test whenever you like without having to fast. Diabetic conditions are indicated by blood glucose levels of 200mg/dl or above.
3) A/C test: Although the A/C test requires blood, you don`t have to fast before having it done. Your medical practitioner will learn from the results. what your typical glucose level has been during the previous two to three months. According to the american diabetes association, your A/C is in the non- diabetes range if it is 5.6% or lower if between 5.7% and 6.4%, pre-diabetes is present. If your result is 6.5% or greater, you likely have diabetes.
How is diabetes managed?
The management of diabetes requires a number of strategies because it is a complex condition. Furthermore, because diabetes has a unique impact on each individual, management strategies must be highly tailored.
The following are the top five(5) components of managing diabetes:
1)Blood sugar monitoring: The effectiveness of your current treatment strategy can be assessed by regularly checking your blood sugar(glucose). It provides you advice on how to take care of your diabetes on a daily and occasionally even on daily basis. With a glucose monitor (CGM) , you can check your levels frequently to track your progress. The ideal blood sugar range for you will be chosen in consultation with your healthcare practitioner.
2)Oral diabetes drugs: Oral diabetes medications assist maintain blood sugar levels in persons with diabetes who still make some use of insulin, primarily those into type 2 diabetes and prediabetes. Oral medications may also be required for those with gestational diabetes.
There are numerous varieties, the most popular drug is metformin
3)Insulin: To maintain their health and control their diabetes, type 1 diabetes must inject synthetic insulin, Insulin may be needed by some type 2 diabetes. There are numerous varieties of synthetic insulin. They all begin to work differently and last in your body for various amounts of time. The four primary methods of ingesting insulin are rapid acting inhaled insulin, insulin pens, insulin pumps, and injectable insulin with a syringe(shot).
4) Diet: Considering how significantly food affects blood sugar levels, meal planning and selecting a balanced diet and important components of managing diabetes. An important aspect of managing diabetes if you take insulin is keeping track of the carbs in your diet. Your need for insulin during meals is influenced by the quantity of carbohydrates you consume. Additionally, healthy diet can lower your chance of developing heart disease and help you control your weight.
5)Exercise: Since exercise improves insulin sensitivity(and lowers insulin resistance),it is crucial for all diabetes to regularly engage in physical activity. As a result of the elevated risk for heart disease, its also critical to keep healthy;
1)Weight.
2)Cholesterol.
3)Blood pressure.
Importance of HbA1c in diabetes management.
Measuring your fasting and random blood sugar is not enough to check on your diabetes. Although, monitoring blood glucose levels when fasting and after meals is crucial, these tests can only measure your blood sugar at a specific period. Depending on what you ate the night before or at the proceeding meal, your findings may differ. The HbA1c test however examines the 3-month data.
HbA1c values for people with diabetes provide a good indication of how well their diabetes is controlled. According to scientific data, a lower Hba1c value indicates a lower risk of developing diabetic complications. Raised Hba1c values in individuals with or without diabetes have also been recognized as a stand alone risk factor for heart disease and stroke.
An Hba1c test requires no specific preparations, unlike fasting or past meal blood sugar. No need to observe a fast. Any time of day is acceptable for providing a test sample.
In general, HbA1c levels typically be checked every three months in persons with diabetes and pre-diabetes. An HbA1c test should be performed every six months, if you are healthy but have a family history of diabetes or believe your lifestyle makes you more likely to acquire diabetes. The frequency of your medical tests can be determined by controlling a health practitioner
.
Prevention of Diabetes.
Diabetes in its autoimmune and hereditary variants cannot be prevented. But there are several actions you can take to reduce your chance of getting gestational diabetes, type 2 diabetes and prediabetes such as:
1)Embrace a healthy diet.
2)Engage in atleast 3 months workout for 5 days in a week.
3)Work toward achieving a healthy weight.
4)Stress management.
5)Consume alcohol in moderation.
6)Get enough rest(usually 7-9 hours) and seek help if you have issues sleeping.
7)Stop using Tobacco.