Uterine Fibroid
Fibroids are tumors made of smooth muscle cells and fibrous connective tissue. They develop in the uterus. It is estimated that 70 to 80 percent of women will develop fibroids in their lifetime, however, not everyone will develop symptoms or require treatment.
Uterine fibroids are the most common tumor of the reproductive tract.
Women who are nearing menopause are at the greatest risk for fibroids. Fibroids are most often found during a routine pelvic exam.
Types of Fibroids
Along with the size and number of fibroids, the type can also affect treatment recommendations. The three main types of fibroids include:
? Subserosal fibroids: These are the most common fibroids. They can push outside of the uterus into the pelvis. Subserosal fibroids can grow large at times and sometimes have a stalk that attaches to the uterus (pedunculated fibroid).
? Intramural fibroids : These fibroids develop in the muscular wall of the uterus.
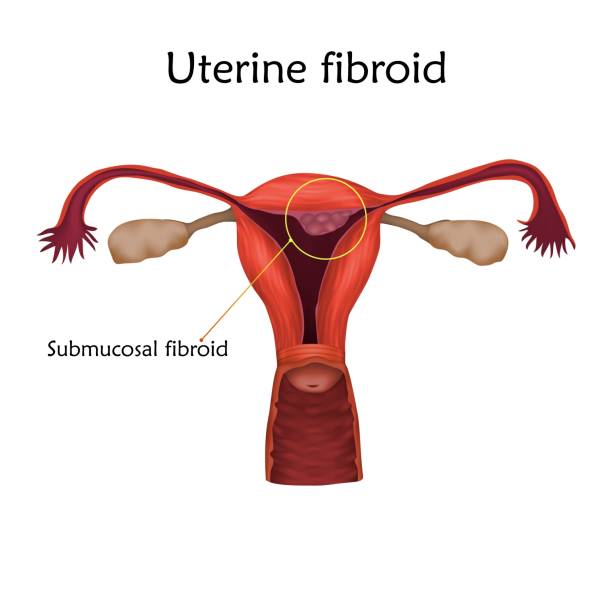
? Submucosal fibroids: These fibroids are uncommon. They can grow into the open space inside the uterus and may also include a stalk.
?There are several risk factors that can play a role in your chances of developing fibroid .
? Obesity.
? Family history.
? Not having children.
? Early onset of menstruation.
? Late age of menopause.
Symptoms of uterine fibroids
Most women with fibroids will experience no symptoms at all. However, large or numerous fibroids can cause the following symptoms:
?Heavy or prolonged periods.
?Bleeding between periods.
?Pelvic pain and pressure
?Frequent urination
?Low back pain
?Pain during intercourse
?Difficulty getting pregnant
Uterine fibroids diagnoses
Fibroids are most often found during a physical exam. Your health care provider may feel a firm, irregular (often painless) lump during an abdominal or pelvic exam.
Scans can confirm a diagnosis. These tests are the two main options:
Ultrasound : Ultrasound is the most commonly used scan for fibroids. It uses sound waves to diagnose fibroids and involves frequencies (pitch) much higher than what you can hear. A doctor or technician places an ultrasound probe on the abdomen or inside the vagina to help scan the uterus and ovaries. It is quick, simple and generally accurate. However, it relies on the experience and skill of the doctor or technician to produce good results. Other tests such as MRI may be better for other conditions, such as adenomyosis.
MRI : magnetic resonance imaging uses magnets and radio waves to produce images. It allows your provider to gain a road map of the size, number and location of the fibroids. We can also distinguish between fibroids and adenomyosis, which sometimes gets misdiagnosed. We use MRI to confirm a diagnosis and help determine which treatments are best for you. MRI may also provide a better option for related conditions such as adenomyosis.
Other tests include :
– Ultrasonography
– Computed tomography
– Laparoscopy
Medications
At present, gonadotrophin-releasing hormone analogs (GnRHa) are mainly used the size reduction or shrinking of fibroid.
Antifibrinolytics agents (tranexamic acid) Used only during the menstrual cycle, tranexamic acid has been associated with up to a 50% decrease in bleeding in women with menorrhagia.
Nsaids to reduce pain
Surgery
Complications of uterine fibroids
It is uncommon for fibroids to cause severe health consequences. However, women can have heavy bleeding that can lead to dangerous anemia, or lack of red blood cells. Rarely, large fibroids can press on the bladder and the channel (ureter) that sends urine there from the kidney. This pressure can lead to kidney damage. Other complications include infertility and repeated pregnancy loss.
In conclusion : Uterine fibroids are a common concern for women in fertile age . It can cause multiple bleeding and pain symptoms which might have a negative impact on women’s life , influencing there sexual , social and work life.
Written by: Samuel Sobiye.