Skin Infections
PREAMBLE:
The skin, the body’s largest organ, plays a crucial role in safeguarding us from external threats, regulating our temperature, and enabling sensory experiences. Composed of various layers, including the epidermis, dermis, and subcutaneous tissue, it acts as a protective barrier against harmful microorganisms and environmental factors. Furthermore, it houses sensory receptors that allow us to sense touch, pain, and temperature. Additionally, the skin contributes to vitamin D synthesis and serves as a canvas for expressing individuality through its unique characteristics, colors, textures, and markings. A comprehensive understanding of the skin’s complexity and functions is vital for maintaining overall health and well-being.
Skin infections, also referred to as dermatological conditions, encompass a broad spectrum of issues that impact the body’s largest organ, the skin. Skin serves as a protective barrier, maintaining body temperature and contributing significantly to sensory perception. Nonetheless, it is vulnerable to a variety of disorders and illnesses, which can manifest in diverse ways, ranging from minor irritations to serious health problems. These conditions may arise due to genetic factors, environmental influences, infections, autoimmune reactions, or lifestyle choices. Examples of common skin disorders include acne, dermatitis (eczema), psoriasis, ringworm, athlete’s foot, among others. Meanwhile, certain conditions like skin cancer can pose life-threatening risks if not identified and treated promptly.
The successful management and treatment of these conditions frequently necessitate a collaborative approach involving a range of medical experts, including dermatologists, allergists, immunologists, and other health practitioners. Additionally, ongoing advancements in medical research and technology are enhancing our comprehension of skin disorders, resulting in improved diagnostic techniques and innovative therapies. Appreciating the diversity of skin disorders is crucial for preserving skin health, averting complications, and enhancing individuals’ overall well-being. Furthermore, we will delve into various aspects of skin disorders, including their causes, symptoms, treatment options, and preventive measures, all aimed at promoting skin health.
TYPES OF SKIN INFECTIONS:
Skin infections can vary greatly in symptoms, severity, and result from various causes, including bacteria, viruses, fungi, and parasites. Here’s a brief overview of some common types:
1. Ringworm (Tinea Corporis):
– Cause: Fungi called dermatophytes.
– Appearance: Red, itchy, ring-shaped rashes on the skin.
– Transmission: Can spread through direct contact with an infected person or animal or by sharing contaminated items like towels or combs.
– Treatment: Antifungal creams or oral medications prescribed by a healthcare professional.
2. Athlete’s Foot (Tinea Pedis):
– Cause: Fungi thrive in warm, moist environments.
– Symptoms: Itchy, peeling skin on the feet, especially between the toes.
– Transmission: Often spreads in locker rooms and public showers.
– Treatment: Antifungal creams or powders, and good foot hygiene.
3. Jock Itch (Tinea Cruris):
– Cause: Fungi that prefer the groin area.
– Symptoms: Itchy, red rash in the groin and inner thigh area.
– Transmission: Common in athletes and those in humid climates.
– Treatment: Antifungal creams or powders, and keeping the area dry.
4. Yeast Infections (Candidiasis):
– Cause: Candida yeast.
– Symptoms: Redness, itching, and sometimes white discharge, often in warm, moist areas like the genitals or mouth.
– Treatment: These fungal infections are typically not serious but can be uncomfortable and itchy. Treatment usually involves antifungal medications/creams, good hygiene, and keeping the affected area clean and dry.
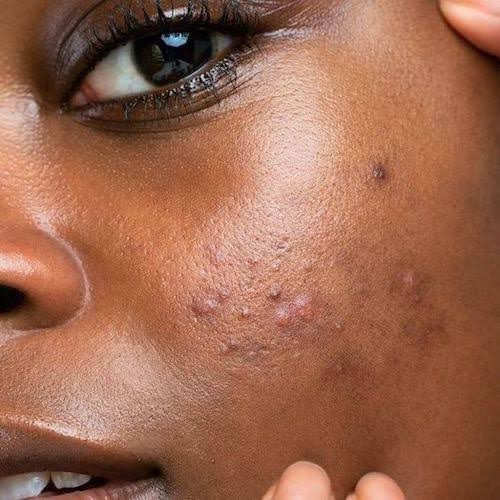
5. Acne:
– cause: Excess sebum production(skin oil), clogged hair follicles, bacteria, hormonal changes, diet, genetics, certain medications (e.g corticosteroids), stress and environmental factors.
– Symptoms: Pimples(small, red, or white bumps on the skin), Blackheads(open clogged pores with dark centers), Whiteheads(closed clogged pores with white centers), Cysts(large, painful lumps under the skin), Inflammation, Scarring.
Treatment:
Acne treatment involves various approaches to manage and reduce the occurrence of acne.
– Cleansing: It’s important to wash your face regularly using a gentle cleanser to eliminate excess oil, dirt, and dead skin cells. Avoid using abrasive scrubs or washing too frequently, as they can cause skin irritation.
– Topical Treatments: Non-prescription products are available and may contain substances like benzoyl peroxide, salicylic acid, or alpha hydroxy acids (AHAs). These ingredients can assist in clearing clogged pores, reducing inflammation, and eliminating the bacteria responsible for acne.
– Oral Medications: In certain situations, healthcare professionals may recommend antibiotics such as doxycycline or tetracycline to reduce inflammation and bacterial growth.
– Chemical Peels: Health practitioners may recommend a visit to certified estheticians for facials like chemical peels to remove the outermost layer of skin, which can improve the appearance of acne scars and promote smoother skin.
– Lifestyle Adjustments: Maintaining a healthy lifestyle through a balanced diet, regular physical activity, effective stress management, and sufficient sleep can have an impact on acne.
– Avoid Picking or Squeezing: It’s crucial to resist the temptation to pop pimples, as this can worsen inflammation and result in scarring.
Keep in mind that treating acne requires patience and consistency. What works for one person may not be effective for another, so it’s essential to consult with a healthcare provider for personalized care. Additionally, some treatments may have side effects, so discussing these with a healthcare professional is important.
6. Dermatitis:
Commonly known as eczema, is a chronic skin condition characterized by inflammation, itching, and sometimes the formation of red, scaly patches on the skin.
Types of dermatitis:
– Atopic Dermatitis: This is the most common form, often appearing in childhood and typically associated with a family history of allergies or asthma.
– Contact Dermatitis: Caused by skin contact with irritants (irritant contact dermatitis) or allergens (allergic contact dermatitis), such as certain soaps, cosmetics, or plants like poison ivy.
Symptoms:
– Intense itching is a hallmark of eczema.
– Redness and inflammation of the skin.
– Dry, scaly, or crusty patches.
– Skin may become thickened or leathery with chronic eczema.
– In severe cases, eczema can lead to open sores or oozing lesions due to scratching.
Causes/Triggers:
– Genetics play a role, as eczema tends to run in families.
– Environmental factors, like exposure to allergens or irritants.
– Dry skin can aggravate eczema.
– Stress and hormonal changes can trigger or worsen flare-ups.
Treatment/Management:
– Moisturizing regularly is essential to keep the skin hydrated.
– Topical corticosteroids and other anti-inflammatory creams or ointments are often prescribed to reduce inflammation and itching.
Prevention:
– Keeping the skin well-moisturized.
– Identifying and avoiding triggers.
– Using mild, fragrance-free soaps and detergents.
– Managing stress, as stress can worsen symptoms.
It’s crucial to understand that eczema is a long-lasting condition without a known remedy, but its signs can be effectively controlled through appropriate skincare, medications, and lifestyle changes. If you or someone you’re familiar with is coping with eczema, seeking advice from a dermatologist or healthcare expert for a tailored treatment plan is recommended.
7. Psoriasis:
This is a long-lasting autoimmune skin condition that impacts millions of individuals across the globe. It arises when the immune system erroneously recognizes skin cells as foreign intruders, prompting an accelerated generation of skin cells. While skin cells typically renew every 3 to 4 weeks, in psoriasis, this renewal process can take as little as 3 to 7 days. This swift turnover of cells results in an accumulation of skin cells on the surface, giving rise to various symptoms like itching, burning, or discomfort in affected areas, as well as dry, cracked skin that may bleed, among other indications. The choice of treatment varies based on the severity and type of psoriasis.
They may include:
– Topical treatments: Creams, ointments, or shampoos containing corticosteroids, vitamin D analogs, or retinoids to reduce inflammation and scale.
– Oral or injected medications: For severe cases, drugs like methotrexate, cyclosporine, may be prescribed to suppress the immune system and reduce symptoms.
– Lifestyle changes: Managing stress, maintaining a healthy diet, and avoiding triggers like alcohol and smoking can help.
– Moisturizers: Using emollients can soothe dry skin and prevent flare-ups. Always consult a healthcare provider for a proper diagnosis and personalized treatment plan.
8. Chickenpox:
This is an infection that causes a skin rash. The disease is caused by a germ called varicella-zoster virus. (Chickenpox itself is also called varicella-zoster.) Most people will get the virus when they are young if they haven’t had a chickenpox vaccine.
A child with chickenpox can easily give the virus to other children. Chickenpox today is much less common because most children are vaccinated when they are young. Having chickenpox once usually provides lifelong immunity to the virus. However, the virus can reactivate later in life, causing a different condition called shingles.
Vaccination:
– The varicella vaccine is highly effective at preventing chickenpox. It’s usually given in two doses to children, and a two-dose regimen is recommended for adults who are not immune to the virus.
Treatment:
– It is mainly focused on relieving symptoms, such as itching and fever, with antihistamines and fever-reducing medications. It’s important to avoid scratching the rash to prevent infection.
SUMMARY:
Various types of skin infections caused by bacteria, fungi, viruses, and parasites exhibit a wide range of characteristics that impact the skin. These infections differ in their origins, symptoms, and therapeutic approaches, underscoring the importance of seeking professional medical advice for precise diagnosis and suitable care. For instance, Pharmacists assume a pivotal role in addressing skin ailments, contributing significantly in multiple aspects. Moreover, they offer vital counsel and proficiency in managing skin conditions by overseeing medication, providing education, and offering patient assistance. Additionally, in cases demanding specialized treatment, pharmacists may refer individuals to dermatologists or other healthcare providers.
Reference:
Google scholar article(complicated infections of skin and skin structures)
Drugs.com
WebMD